Stay updated with expert articles, tips, and stories that inspire and inform
-
June 3, 2026Read more ...
QurCan Therapeutics fosters scientific creativity through pioneering nanotechnologies to discover and develop breakthrough therapeutics, leveraging its proprietary nanoparticle drug-delivery technology, “TERP”. The Goal Update the pitch deck to build credibility, strengthen brand identity, and provide clear value to current and potential investors. The ultimate goal of QurCan is to streamline their fundraising efforts. Visualizing complex
-
June 3, 2026Read more ...
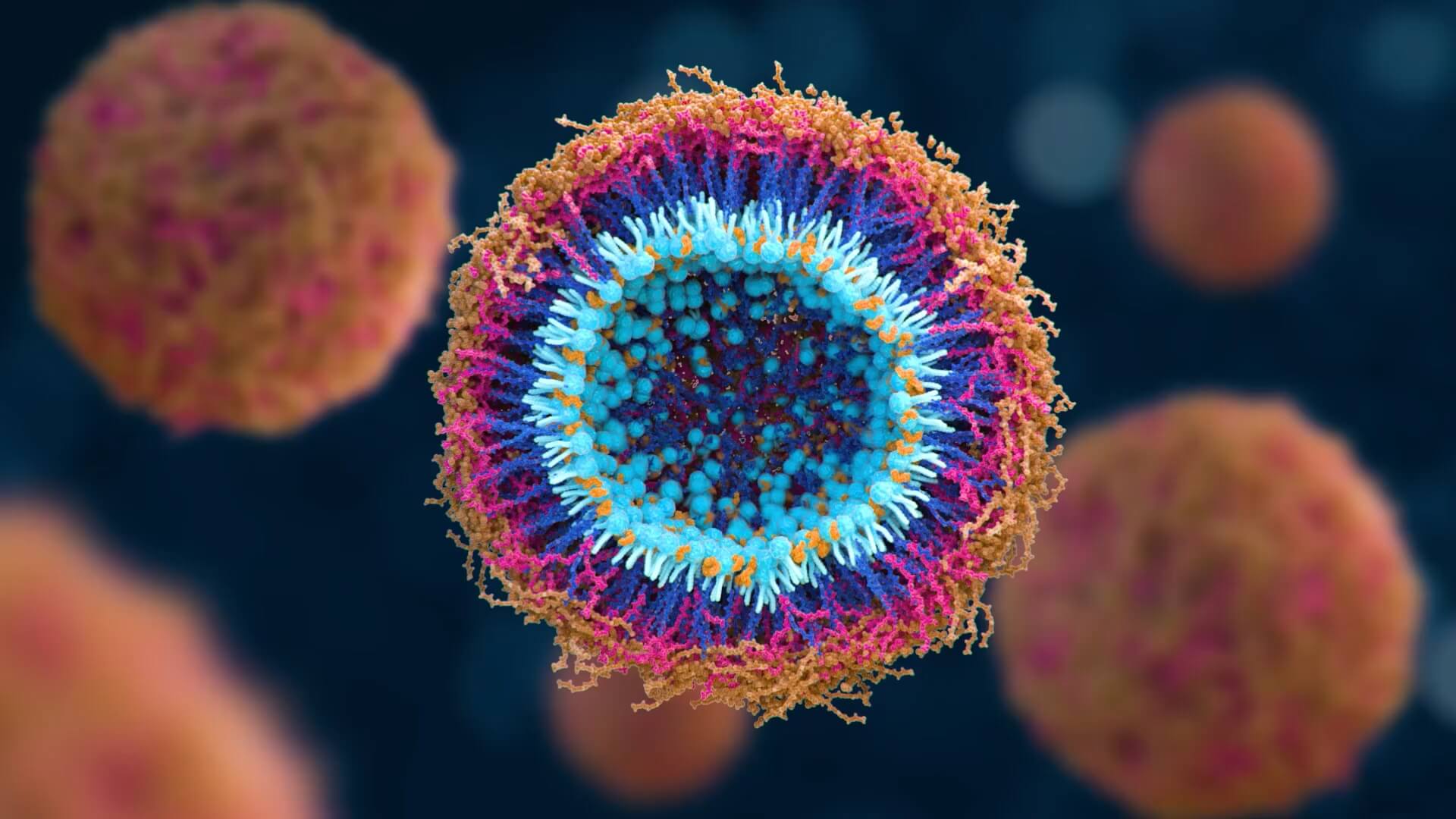
MaveriX Oncology is exploiting new insights into cancer and immune cell metabolism to advance a new generation of Conditionally Activated Small Molecule TherapeuticsTM designed to specifically co-target cancer and the tumor immune microenvironment. The Goal To translate complex scientific concepts into compelling, easy-to-understand visuals that could be used both for fundraising and for enhancing the
-
June 3, 2026Read more ...
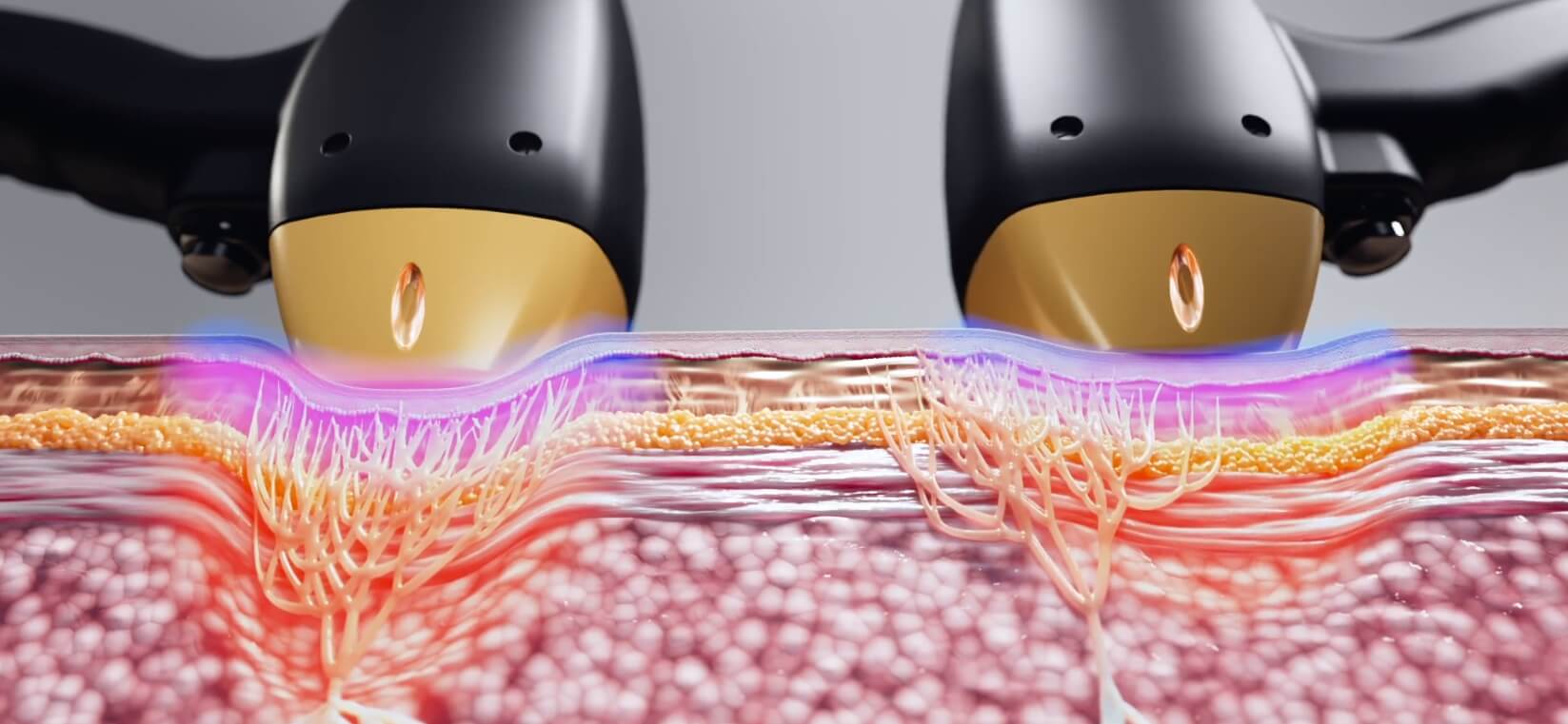
Alma Lasers is a global innovator of laser, light-based, radiofrequency, and ultrasound solutions for the aesthetic and surgical markets. The Goal To demonstrate a transformative approach to dermatology and highlight the advantages of the technologies. Pixel RF 3D animation of RF UniPolar Plasma Technology. Accent Prime 3D animation of the Multi-Platform RF and Ultrasound Device.
-
Read more ...
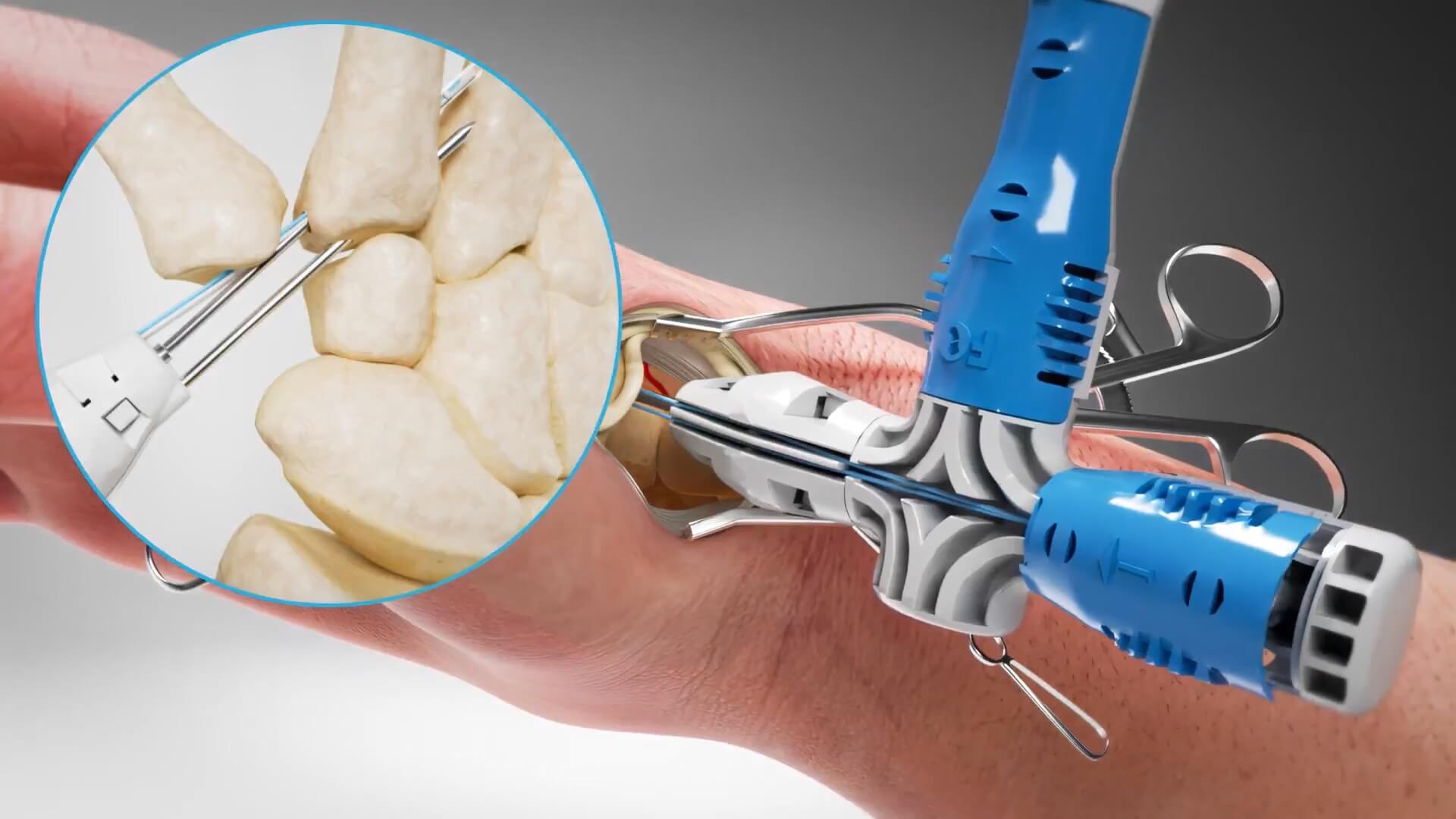
Field Orthopaedics is a medical technology company dedicated to advancing the field of hand surgery through innovation. They specialize in the development of cutting-edge medical implants and surgical solutions that improve outcomes for both patients and surgeons and transform the standard of care in orthopaedic hand procedures. Challenge 3D animation for the demonstration of a
-
October 12, 2024Read more ...
Project scope To showcase expertise in an integrated robotic platform for tissue engineering and developing artificial joints using stem cells and 3D printing. KU Leuven is an international community where innovative research forms the basis of all academic programs. JOINTPROMISE project paves the way for high-volume, affordable production of entire biological joints, addressing a major