Aesthetic medicine companies have to appeal to two distinctively different types of audiences. First, they need to communicate with end consumers of beauty products. These consumers often lack the necessary knowledge about the anatomy and biochemistry of skin, beauty products, and beauty procedures. They need an education that will simplify complex terms and processes and deliver clear-cut, easy-to-understand knowledge.
The second category of consumers consists of businesses that resell or utilize aesthetic products and devices. Decision makers in these companies possess significantly greater knowledge and understanding of dermatology and aesthetic medicine. However, they also experience buyer fatigue and analysis paralysis.
Medical animation can help you boost your communication with potential clients, both end consumers and businesses. In this article, we discuss 5 reasons why you need medical animation.
5 reasons to use medical animation in communication with clients
Medical animation can help dermatology and other aesthetic companies communicate consistently with end consumers and other businesses. In this article, we discuss how these videos can help:
- Boost trust
- Make communication more efficient
- Make messages clear
- Evoke aesthetic emotions
- And assist in marketing efforts
Trust
In her recent publication Consumer Trust in Online Purchase Decision, Mahliza shows how trust positively correlates with the purchasing decision. In the same paper, she also demonstrated the negative impact that perceived risk can have on the buyer’s trust overall.
The perceived risks in various aesthetic procedures and application of beauty products are high. The negative consequences of such procedures or product use can have lasting impacts on both the health and visual representation of the consumer.
According to McDonald and Hedenrych, the qualifications and training of a practitioner were the number one factor for trust. Adams gives similar advice in his article for aestheticmed.co.uk emphasizing the importance of authority in the field.
Scientific animation can help you gain the trust of your consumers by showcasing your knowledge, expertise, and experience in solving their delicate problems.
Check out our case study for Hydrafacial and their Vortex Fusion Technology:
Efficiency of communication
According to Dosher and McBride, pictures play a pivotal role in processing and memorizing information by humans. Videos can enhance the understanding of the message and its recollection even more by using consistent storytelling.
Since animation utilizes three types of information: audio, visual, and text, it can deliver more data to the viewer per second than reading.
Let’s take a look at the video we made for Sturm:
Using visuals it tells a consistent story about the damage human hair experiences from various environmental impacts (sunlight, pollution, styling, etc.) becoming dull and brittle. The video then offers a restorative solution that is consistent with the values of modern society (vegan, cruelty & GMO-free) and doesn’t contain questionable chemicals (PEGs and Paraben). The viewer can witness the hair restoration.
When communicating with professionals, the efficiency of communication is as important. Yours isn’t the first salesperson who tries to sell injections to a dermatology clinic. 50-second medical animation demonstrating the benefits of your product can save their time on listening to your sales pitch, spark genuine interest, and help stand out.
Check out our case study for SoftFil® PRECISION cannulas:
Clarity
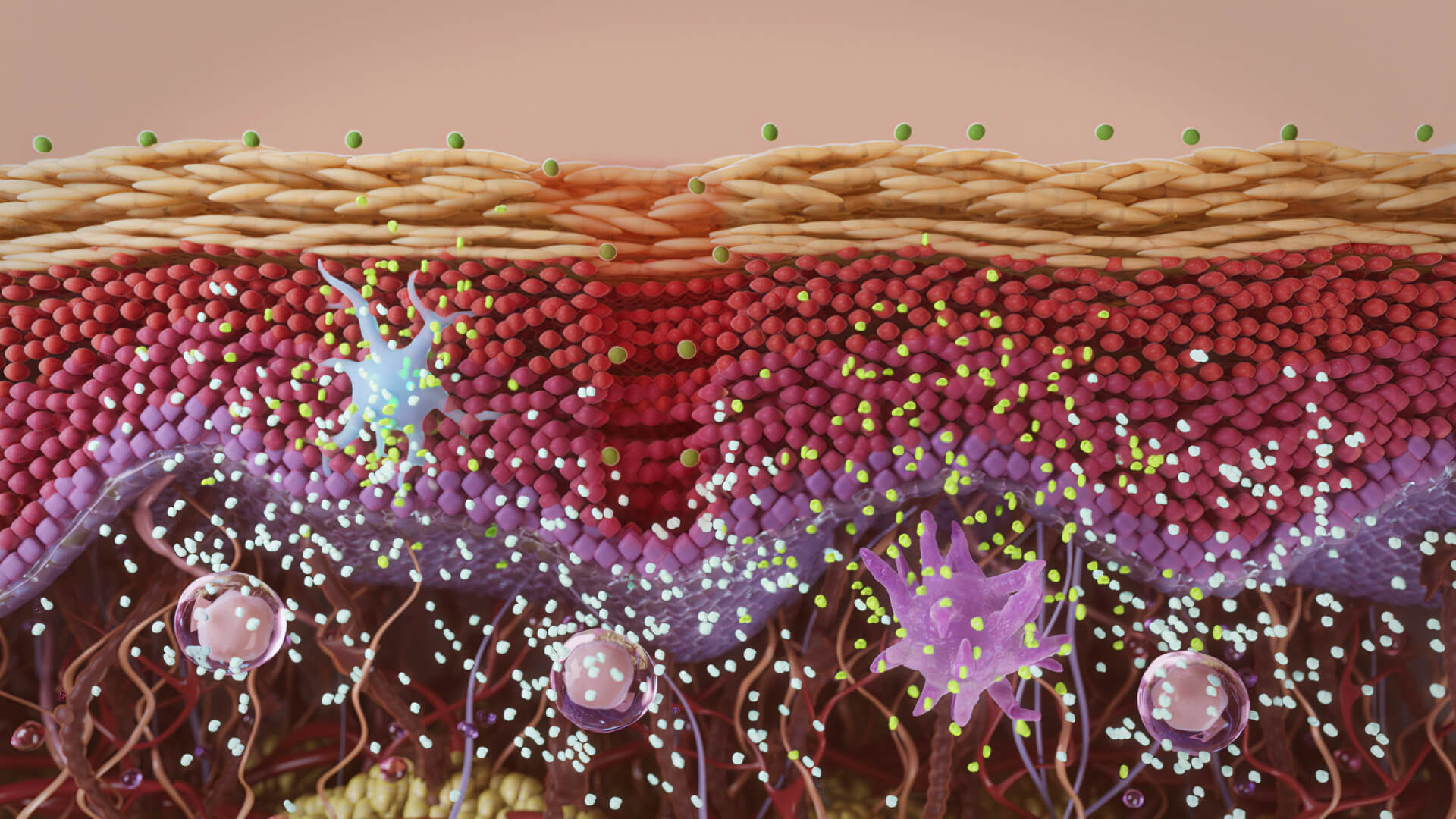
One of the greatest challenges that aesthetic medicine businesses face in promoting their products or services is educating potential and existing clients. The anatomy and biochemistry of human skin is complex. Meanwhile, the level of scientific knowledge of most consumers is mostly insufficient for understanding modern cosmetology.
A long text with medical terminology that depicts cellular processes can exhaust even fellow dermatology professionals, let alone mere consumers.
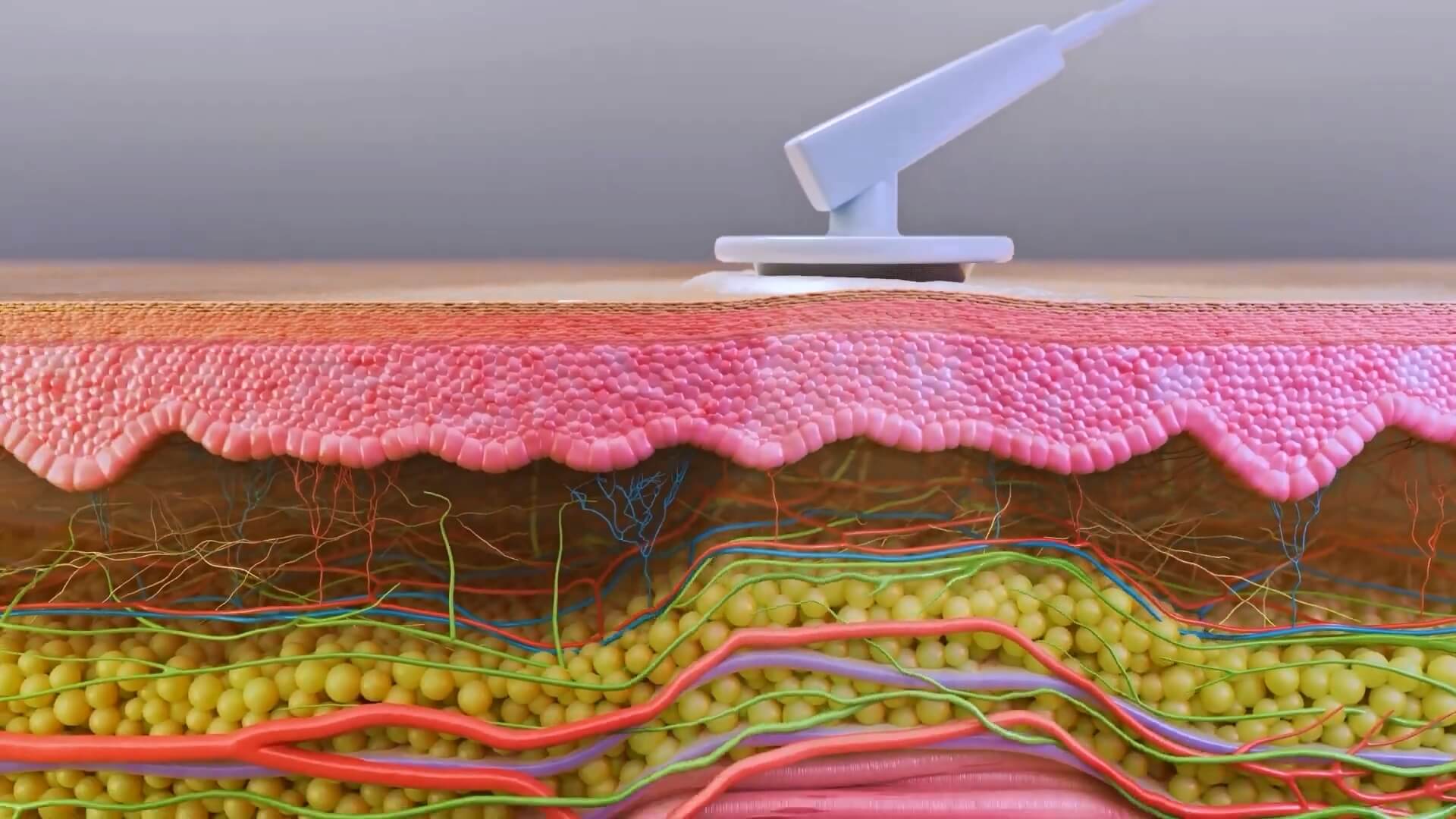
Scientific animation, on the other hand, can visualize skin at tissue or even cell level. It can depict the damaging processes like aging as well as restoration provided by a product or procedure.
Here’s an example of a medical animation that visualizes how radiofrequency technology and micro-needling can impact skin on a tissue level:
Aesthetics
According to Hagtvedt, aesthetics play an important role in marketing and selling products. However, it is even more important when it comes to marketing beauty procedures and products.
We’ve already established that animation can turn complex anatomical and biochemical info-dump into an engaging narrative. Now, we want to emphasize the importance of the visual appeal of videos to the communication with your consumer.
Armstrong and Detweiler-Bedell successfully argued that experiencing pleasure from beauty is an emotion as opposed to cognitive processing. That’s why aesthetically pleasing animation can help the consumer to emotionally connect with complex educational information accompanying beauty products and procedures.
Furthermore, the depiction of unpleasant skin conditions like acne or wrinkles removed, i.e., the beautifying process can significantly enhance the emotional impact and facilitate decision-making.
Check out how in just several seconds viewers can witness the reversion of skin aging, reduction of acne, and moisturizing of the skin:
Marketing & Promotion
Scientific animation can benefit the marketing and promotion efforts of your company in several ways:
1. Conversions
The reported increase in conversion rates from utilizing video fluctuates between 80% and 144%. These figures depend on the industry, video, position on a page, medium, sales cycles, and a plethora of different other factors.
2. Omnichannel approach
Like any type of content, medical animation can be repurposed for various types of mediums providing consistent communication with the client. The mediums include YouTube channels, websites, presentations, brick-and-mortar shops, booths at conferences, influencers, etc.
3. Business Development
Some companies use scientific animation for business development as it can help owners explain to potential partners and investors what the company does. Additionally, investors often assess a firm’s marketing efforts among other factors.
4. B2B
Many companies provide medical animation for their clients to place on their websites and other media. A great video that explains the benefit of a product or procedure to the end consumer can be a benefit in negotiating a deal with a clinic or a distributor. It will be appealing to purchase a product with marketing materials that can help promote it.
5. SEO
Google loves visual content. It pushes the pages with visuals higher on SERP in case your content is relevant and optimized. But that’s not all. People are more likely to share a link to your videos with others or publish your videos in their blogs boosting your domain authority. People will stay longer on your page if there is a video there, signaling to Google that this page has relevant information.
Wrapping up, medical animation can help you establish trusting relations with your potential clients, communicate with them in a clear and consistent way, and boost your promotional and marketing efforts.